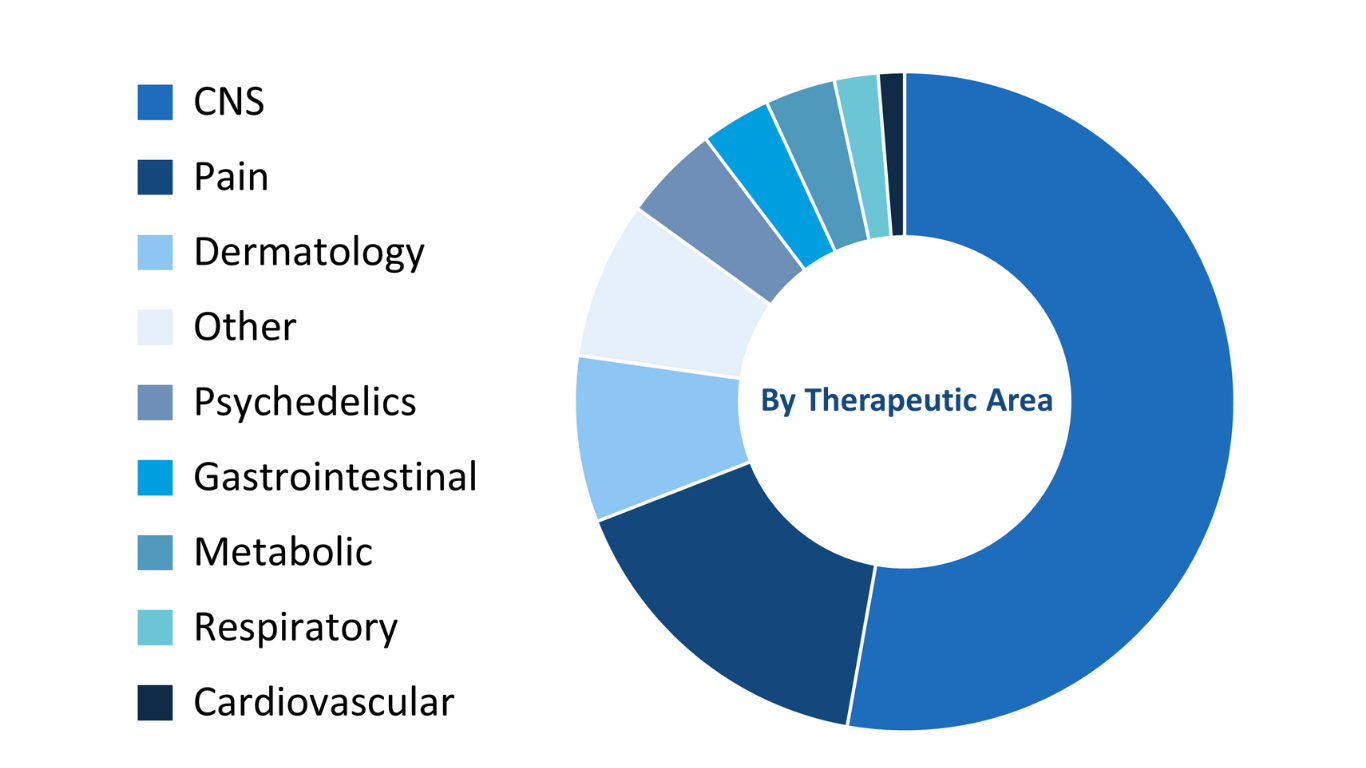
The placebo response or the placebo effect. We hear about it a lot, but what happens in practise? Let’s unravel it by understanding what it actually is. The “placebo effect” occurs when a person who is ill perceives an improvement, or actually experiences an improvement, in symptoms or overall health from the psychological effect of receiving treatment, rather than from the treatment itself.
Alarmingly, the magnitude of placebo response is growing in clinical trials. In the US in 1996, 27% of patients showed pain reduction when given pain drugs in clinical trials. When similar studies were run in 2013, only 9% showed pain reduction.

MAC’s Chief Scientific Officer, Dr. John Connell, voices his concerns, saying that “the reason for this is not that drugs are becoming less effective, it is because people on ”dummy drugs” are getting better probably due to psychological reasons. How a person responds to treatment is part pharmacology and part psychology. This may be influenced by experience with previous treatments, trust in the clinician, information on social media, and many other factors.”
As clinicians and scientists, we have a responsibility to reduce the placebo effect as we cannot separate it from drug effectiveness, which may lead to potential game-changing treatments being stopped in error.
Dr. Connell leads MAC’s Scientific Solutions offering. Services include psychological assessments, human models of disease, and placebo training for staff and patients. Dr. Connell’s team have noticed many factors that influence treatment response, such as:
- Positive mental attitude
- Trust in the clinical study team
- Increased medical attention while participating in a study
- Social media and press reports on the condition or treatments
- Interaction with other patients in the study
- Previous experience with medications
The challenge for site and Sponsor teams is that ALL of these elements must be controlled in clinical studies.
At MAC we achieve this using a three-pronged approach. First, we train site staff around the world to be aware of the dangers of causing an increased placebo response; and steps that can be taken to minimise effect. Second, we make sure patients know how to report key study endpoints consistently and reliably. And finally, we train study participants on the importance of accurate reporting of their condition at all times. This helps our study teams avoid speculation on trial effects and helps manage participant and team expectations of the study treatment.
Our approach is novel: not all CROs offer this type of education and training to both study staff and patients. Of course, through the COVID-19 pandemic we had to adjust to virtual training, but now we offer a choice of either in-person or virtual training, and certainly notice that in-person training for all site staff proves more effective than training via video or phone call platforms.
Using this approach, MAC has successfully managed the placebo response in many studies across multiple countries and sites.